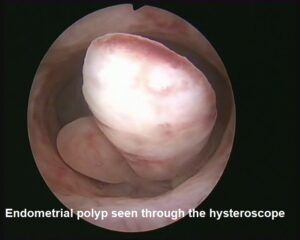
 The hysteroscope is a small lighted telescope used for visual examination of the cervix and the uterus to help diagnose and treat abnormalities in the cervical canal or the uterine cavity. If it is used to look for the cause of the presenting problem, it is term as diagnostic hysteroscopy. If it involves some form of surgical procedures such as removal of growths (endometrial polyps or fibroids), removal of the lining or separation of adhesions, then it is called operative hysteroscopy. In many cases, both procedures are done concurrently – the so-called “see and treat” approach.
The hysteroscope is a small lighted telescope used for visual examination of the cervix and the uterus to help diagnose and treat abnormalities in the cervical canal or the uterine cavity. If it is used to look for the cause of the presenting problem, it is term as diagnostic hysteroscopy. If it involves some form of surgical procedures such as removal of growths (endometrial polyps or fibroids), removal of the lining or separation of adhesions, then it is called operative hysteroscopy. In many cases, both procedures are done concurrently – the so-called “see and treat” approach.
Reasons for the procedure
- Evaluation and treatment of abnormal uterine bleeding.

- To look for the displaced and removal of the intrauterine device (IUD).
- Evaluation for infertility (difficulty in conceiving) or recurrent miscarriage.
- Uterine polyps, fibroids or adhesions (which is called Ashermann’s syndrome).
- Obstructed fallopian tubes.
- Congenital malformations of the uterus
Preparation for the procedure
Ideally, it is best to schedule the procedure following completion of menstrual flow when the lining is at its thinnest. However, this is sometimes not possible, especially when it is done for abnormal uterine bleeding. It can be done either as an
- Out-patient procedure, without any anaesthesia or analgesia – this is possible because of the small caliber of the hysteroscope and no cervical dilatation is required. Therefore, this will reduce discomfort significantly. Fasting is not required. However, it is not advisable to take a full meal just prior to the procedure.

- Day-case procedure, usually under a light general anaesthesia. You are required to fast for at least 6 hours before the procedure (no food or drinks at all for 6 hours). For example, if the procedure is in the morning, you should skip breakfast. If it is in the afternoon, you can have an early light breakfast (e.g. tea/coffee/milo and toast) but make sure that this is taken at least 6 hours before the procedure. Please reconfirm this with your doctor.
Description of procedure
- It is sometimes performed in combination with a laparoscopy.
- The hysteroscope is passed through the vagina and cervix into the uterine cavity for viewing. Saline fluid is used to distend (expand) the uterine cavity to improve visualization and allow any operative manipulations to be achieved. Video monitoring is often used at the same time.

- For operative hysteroscopy, a variety of small surgical instruments are available for use in hysteroscopic procedures including scissors, special clamps, or wire with electro-cautery attachment for coagulation and cutting. One attachment is a “rollerball” or wire loop through which electrical heat travels to remove (resection) the fibroid or endometrial lining. After the uterus is filled with fluid to enlarge it for better viewing, the doctor moves the roller¬ball back and forth across the lining or uses the wire loop to shave off the tissue. This method is called endometrial ablation. The wire loop can be used to remove the submucous type of fibroids. This is called hysteroscopic resection of fibroid.
- The hysteroscope is then withdrawn.
Complications
For diagnostic hysteroscopy, the risk of is very low. This includes uterine perforation or excessive bleeding. For operative hysteroscopy, the complication rate is slightly higher and includes:
- Pelvic infection.
- Cervical trauma due to dilatation and manipulation during surgery
- Excessive fluid absorption into the blood circulation.
Post-procedure care
If performed as an office procedure without any anaesthesia – the recovery is immediate. You will be allowed home as soon as you have finished the consultation with your doctor. It is best if you have someone to drive you home.
If performed as day-case under general anaesthesia:
- Following the procedure, your vital signs will be monitored for a period of time.
- Once the anaesthetic effect has wear off and you are fully awake, you will be allowed to go home.
 Please arrange for someone to drive you home.
Please arrange for someone to drive you home. - There may be some slight bleeding and cramping. The fluid used during the hysteroscope will flow out for one to two days. Use sanitary napkins—not tampons—to absorb blood or drainage.
- Antibiotics may be prescribed prior to and after the procedure to prevent infection. This is uncommon and usually not required.
- Medicine for pain may be given during or after the procedure.
- Rest at home during the remainder of the day. Additional restrictions may be required depending on the extent of the surgical procedure.
- Avoid sexual intercourse for 2 weeks or as directed.
- There is no special dietary restrictions.
See your doctor immediately if there is:
- Excessive bleeding.
- Abnormal vaginal discharge.
- Increasing abdominal pain or abdominal distention
- Signs of infection develop, such as headache, muscle aches, dizziness or a general ill feeling or fever.









