 A myomectomy is the removal of fibroids (leiomyomas, myomas) from the uterus. Patients can have a single or numerous fibroids. Myomectomy treatment for fibroids preserves the uterus. It is most often recommended to women who desire future pregnancy or wishes to retain her uterus. A patient undergoing the myomectomy procedure should be informed regarding the risk of hysterectomy. This may be necessary if excessive bleeding occurs, or if it is not possible to reconstruct the uterus because of the many defects left by the removal of multiple small fibroids or a single large fibroid.
A myomectomy is the removal of fibroids (leiomyomas, myomas) from the uterus. Patients can have a single or numerous fibroids. Myomectomy treatment for fibroids preserves the uterus. It is most often recommended to women who desire future pregnancy or wishes to retain her uterus. A patient undergoing the myomectomy procedure should be informed regarding the risk of hysterectomy. This may be necessary if excessive bleeding occurs, or if it is not possible to reconstruct the uterus because of the many defects left by the removal of multiple small fibroids or a single large fibroid.
REASONS FOR PROCEDURE
- Significant pelvic pain or back pain.
- Large size or rapidly growing.
- Anemia caused by excessive loss of blood (abnormal uterine bleeding).
- Pressure on the bladder or the rectum.
- Difficulty in becoming pregnant.
- Discomfort with sexual intercourse.
- Pregnancy complications due to the fibroids.
DESCRIPTION OF PROCEDURE
 Abdominal myomectomy is an in-patient open surgery procedure. A general anaesthetic will be administered.
Abdominal myomectomy is an in-patient open surgery procedure. A general anaesthetic will be administered.
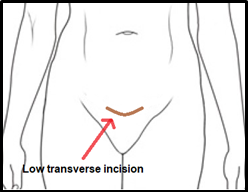
- The incision to enter the abdominal cavity is similar to the procedure for Caesarean delivery, which is a transverse incision at the lower abdomen. In some women with large and multiple fibroids, a midline incision below the navel (umbilicus) may be required.
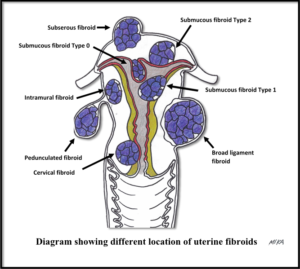
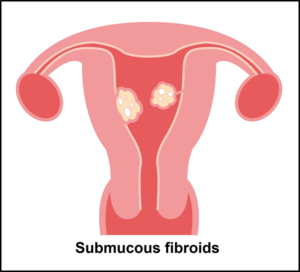
- Types of fibroids are determined by location in the uterus. Subserous appear on the outside of the uterus, intramural is confined to the wall of the uterus, and submucous appear inside the uterus. Rarely, fibroids can involve the cervix.
- Each fibroid is removed separately, and each uterine incision is repaired with absorbable sutures.
- An adhesion barrier can be placed over the uterine incisions to prevent adhesion formation.
- The abdominal layers are closed in layers.
- The skin is closed with absorbable or non-absorbable sutures.
 Laparoscopic myomectomy uses a telescopic instrument (laparoscope) which is inserted through the navel to do the operation. The advantages of laparoscopic myomectomy are less pain after surgery, less chance of adhesions, reduced risk of infection, reduced risk of blood clots in the legs or lungs, a shorter hospital stay and a quicker recovery.
Laparoscopic myomectomy uses a telescopic instrument (laparoscope) which is inserted through the navel to do the operation. The advantages of laparoscopic myomectomy are less pain after surgery, less chance of adhesions, reduced risk of infection, reduced risk of blood clots in the legs or lungs, a shorter hospital stay and a quicker recovery.
- General anaesthetic is administered
- The bladder is emptied with a catheter
- It is often necessary to insert an instrument called uterine manipulator through the vagina and cervix into the uterus in order to help move the uterus around.
- A small incision is made in or below the patient’s navel. A needle is inserted to inflate the abdomen with carbon dioxide. The laparoscope is then inserted to view the abdominal and pelvic cavity.
 It is connected to a high intensity light and a high-resolution television camera so that the doctor can see the abdominal and pelvic organs. Additional instruments will be placed near the laparoscopic port and used to perform the myomectomy. Each fibroid is removed separately, and each uterine incision is closed with sutures using these instruments.
It is connected to a high intensity light and a high-resolution television camera so that the doctor can see the abdominal and pelvic organs. Additional instruments will be placed near the laparoscopic port and used to perform the myomectomy. Each fibroid is removed separately, and each uterine incision is closed with sutures using these instruments. - Fibroids will be removed using a morcellator. See below for further discussion on morcellation.
- At the end, the laparoscope is removed, and the carbon dioxide is allowed to escape from the abdomen. The uterine manipulator is then removed
- Absorbable sutures are used to close the wound.
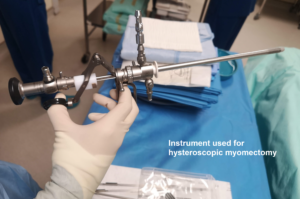
Hysteroscopic myomectomy uses a special type of hysteroscope called a resectoscope This instrument has a built-in wire loop and uses electrical current to cut out the fibroids into small pieces. This method is used to remove the type of fibroid that grows within the uterine cavity (called the submucous type). There is no surgical incision or skin scarring. Postoperative recovery is also quicker, with no or very minimal pain. It is often done as a daycare procedure and you can go home on the same day
EXPECTED OUTCOME
- The uterus is left intact, and you will still have menstrual periods. Your next period should occur at about the expected time.
- Symptoms such as heavy bleeding and pressure discomfort usually decrease or are gone once the fibroids are removed.
- Fertility will improve if the fibroid is the direct cause. However, pregnancy should be avoided for at least 6 to 9 months to allow for uterine wound healing. Please discuss with your doctor for more details. A contraceptive plan is important as well (family planning method to avoid pregnancy during this period)
POSSIBLE COMPLICATIONS DURING SURGERY
- Excessive bleeding; rarely, may necessitate a hysterectomy, which is the removal of the uterus (1% risk)
- Adjacent organ injuries during surgery (such as bowels or bladder)
- Conversion of either the laparoscopic or hysteroscopic approach to an open abdominal surgery due to complications.
- Surgical-wound infection.
- Development of adhesions between the uterus and other pelvic structures. This risk can be reduced by using adhesion barrier.
POSSIBLE COMPLICATIONS AFTER SURGERY
- A myomectomy carries a risk of potential pregnancy-related complications. Disorders of the placenta or weakness in the uterine wall may occur. In certain myomectomy procedure, you may not be allowed for vaginal delivery due to higher risk of uterine rupture during labour. An elective caesarean section is a safer alternative and your doctor will discuss this with you after the operation.
- Recurrence of the fibroids.
BEFORE THE OPERATION
- A hormone injection such as the gonadotropin-releasing hormone (GnRH) agonist may be given before surgery. It is usually given as a monthly injection for 2 to 3 months. This hormone will block the production of oestrogen and progesterone, thereby stopping the menstruation. In a woman with low haemoglobin before surgery, this will be helpful in raising the iron store and the haemoglobin level, thus avoiding an unnecessary blood transfusion. It will also help to shrink the fibroid size and maybe helpful during the surgery.

- Consent for operation should be signed.
- Relevant investigation that may be taken will depends on your medical illness and age. This may include blood tests, ECG (electrocardiogram) and chest X-ray.
- You are required to fast for at least 6 hours before surgery (no food or drinks at all for 6 hours). For example, if the surgery is in the morning, you should skip breakfast. If it is in the afternoon, you can have an early light breakfast (e.g. tea/coffee/milo and toast) but make sure that this is taken at least 6 hours before the surgery. Please reconfirm this with your doctor.
POSTOPERATIVE CARE
Abdominal Myomectomy
- Hospital stay is usually 2 to 4 days
- Fever is common during the 48 hours after surgery.
- Food is not allowed immediately following the surgery. Fluids will be given via an intravenous line. Your doctor will review periodically to decide when to start orally. Initially, only clear liquid diet is allowed, and if you can tolerate it, then you will be given nourishing fluid and followed by a soft diet. You should eat a well-balanced diet to promote healing.
- There may be a urinary catheter in the bladder to allow drainage of urine and is usually removed the following day.
- Pain relief medication will be given via injection and later change to an oral tablet.
- Antibiotic is given at time of operation and may be continued if there is a risk of infection.
- It is important to mobilize as soon as possible, since it helps prevent complications, such as blood clots and pneumonia.
- Getting up from bed on the following day – it is easier if you roll to your side at the edge of the bed. Put your head on your elbow, then slowly dropping both legs over the side of the bed. At the same time, slowly push yourself up sideways with your elbow and sitting up slowly into a sitting position. Try to use the other hand for support by crossing it over your body. Sit for a while on the bed to get your balance and then slowly stand up. You can do the opposite to get back into bed (in reverse order). By using this method, you will put less pressure on the stitches and abdomen.
- Gas pain (abdominal wind) can be a problem following the operation for some women. Early mobilization will help to reduce the wind. If the problem persists, medication can be prescribed for relief.

- Wound inspection is done before discharge and a new waterproof dressing is applied. Upon discharge, follow-up visit will be scheduled at day 7 or 8.
- Once home, someone should be available to help care for you for the first few days.
- Shower as usual.
- Non-absorbable sutures are usually removed from the skin incision on the seventh day. If absorbable suture is used, then the suture need not be removed. It will dissolve by itself after a few weeks.
- Expect some soreness around any incision site; this is normal. A firm ridge may form along the incision. As it heals, the ridge will recede gradually. After 1 week, you may wash the incision gently with mild soap and wipe dry the area with a clean dry towel.
- Slight vaginal bleeding may occur after surgery. Use sanitary pad and not tampons for this purpose.
- To help recovery and aid your wellbeing, resume daily activities, including work, as soon as you are able. Heavy lifting and strenuous activity should be avoided. Recovery at home may take 2 to 3 weeks, with full activities resumed in 4 to 6 weeks. Incisional numbness, occasional aches and pains may last for another few weeks.
- You can resume driving after 3 to 4 weeks, provided full mobility has returns and painkillers medications are no longer required. Please ask your doctor if you are not sure.
- Sexual relations may be resumed in 4 weeks.
Laparoscopic Myomectomy,
- Hospital stay is shorter, and recovery is faster.
- You will be allowed fluid intake after surgery if there is no nausea or vomiting. Soft diet is usually given the next day.
- There may be a urinary catheter in the bladder to allow drainage of urine and is usually removed the following day.
- Pain relief medication will be given via injection and later change to oral tablet.
- Antibiotic is given at the time of operation and may be continued if there is a risk of infection.
- It is important to mobilize as soon as possible, since it helps prevent complications, such as blood clots and pneumonia,
- You may experience slight discomfort for 24 to 48 hours. You may have aches in your shoulders and chest from the carbon dioxide that was used to inflate your abdomen. No treatment is necessary.
- Gas pain (abdominal wind) can be a problem following the operation for some women. Early mobilization will help to reduce the wind. If the problem persists, medication can be prescribed for relief.
- Upon discharge, follow-up visit will be scheduled on day 7 or 8.
- Absorbable suture is often used. Therefore, the stitches need not be removed.
 Hysteroscopic Myomectomy, there is no surgical incision. The post-operative recovery is the fastest and with the least pain or no pain at all. This is usually done as a daycare. The patient can be allowed to go home a few hours after the procedure. Oral painkiller will be given for you to take home. You can shower as usual. Most women can return to work within a few days and back to normal activity a week later (including driving). Vaginal bleeding and later pinkish watery vaginal discharge is present for 2 to 3 weeks. Use sanitary napkins—not tampons—to absorb blood or drainage and avoid douching, swimming, and baths till no more vaginal discharge. Sometimes, the fibroids may be incompletely removed at the first attempt due to the large size or excessive absorption of the fluid that was used during surgery. In such a case, the hysteroscopy is usually scheduled again in 4 to 6 weeks to complete the myomectomy.
Hysteroscopic Myomectomy, there is no surgical incision. The post-operative recovery is the fastest and with the least pain or no pain at all. This is usually done as a daycare. The patient can be allowed to go home a few hours after the procedure. Oral painkiller will be given for you to take home. You can shower as usual. Most women can return to work within a few days and back to normal activity a week later (including driving). Vaginal bleeding and later pinkish watery vaginal discharge is present for 2 to 3 weeks. Use sanitary napkins—not tampons—to absorb blood or drainage and avoid douching, swimming, and baths till no more vaginal discharge. Sometimes, the fibroids may be incompletely removed at the first attempt due to the large size or excessive absorption of the fluid that was used during surgery. In such a case, the hysteroscopy is usually scheduled again in 4 to 6 weeks to complete the myomectomy.
SEE YOUR DOCTOR IMMEDIATELY IF THERE IS:
- Increasing pain, swelling, redness, discharge, or bleeding in the surgical area.
- Vaginal bleeding which soaks more than 1 pad each hour.
- The urge to urinate frequently, especially if associated with pain and abnormal urine colour.
- Persistent and abnormal vaginal discharge.
- Increasing nausea and vomiting, with or without abdominal distention. Poor oral intake
- Short of breath or feel faint.
- Signs of infection, including headache, muscle aches, dizziness or a general ill feeling and fever.
Laparoscopic myomectomy and morcellation
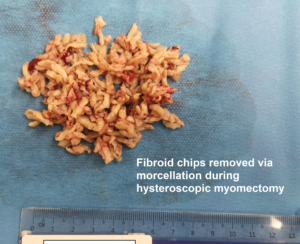 Morcellation is when the fibroids are cut into smaller pieces to allow them to be removed more easily. This can be done using an instrument called a morcellator which electrically or mechanically cuts the tissue into smaller pieces. Morcellation is often used in laparoscopic myomectomy to assist the removal of the fibroids through a small incision.
Morcellation is when the fibroids are cut into smaller pieces to allow them to be removed more easily. This can be done using an instrument called a morcellator which electrically or mechanically cuts the tissue into smaller pieces. Morcellation is often used in laparoscopic myomectomy to assist the removal of the fibroids through a small incision.
Risks of morcellation includes:
- Small pieces of benign (non-cancerous) fibroid tissue could be left inside your abdomen during the morcellation. These may then attach to the internal organs in your abdomen where they can continue to grow and may require another surgery in the future to remove it. The risk of this happening is thought to be 1 in 120 (uncommon) to 1 in 1200 (rare).
- There is a chance of an unexpected uterine sarcoma (a cancerous type of fibroid) and the use of morcellation in this situation may cause the cancer to spread during the surgery and worsen your chance of survival. The risk of unexpected uterine sarcoma in fibroids depends on your age and is higher in older women. Various studies have quoted this risk as ranging from:
- 1 in 304 to 1 in 1250 (if you are younger than 50).
- 1 in 158 to 1 in 303 (if you are between 50 and 59)
- 1 in 65 to 1 in 278 (if you are over 60 years of age),
There are certain clinical and ultrasound scan findings plus the presence of risk factors that can raise suspicion that the fibroids may be of a cancerous type. In this situation, your doctor may offer open surgery where a larger cut is made on your abdomen to remove your fibroids or uterus. The risks and benefits of laparoscopic (with morcellation) and open surgery will vary depending on your individual situation such as the numbers and size of fibroids, need for fertility, probability of uterine sarcoma and your preference. These will be fully discussed with you by your healthcare professional.
View this post on Instagram
For further reading:
Information for You: Morcellation for myomectomy or hysterectomy – Published in October 2019 by RCOG UK
To download a pdf copy, CLICK HERE
To read more about fibroids, click HERE
CLICK HERE to view images of gross specimens of fibroids after surgical removal
CLICK HERE to view videos on laparoscopic myomectomy
CLICK HERE and HERE to view videos on hysteroscopic myomectomy