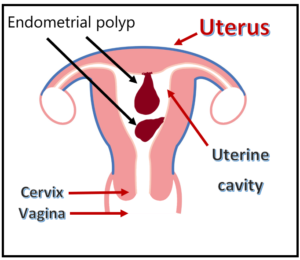
 Endometrial polyps are growths that arise from the inner walls that lined the uterine cavity. It is sometimes called uterine polyps. It is believed to arise from the overgrowth of endometrial tissue. It may range in size from a few millimetres only to a few centimetres. Sometimes, there can be several polyps present at the same time. It may have a long stalk and can extends through the cervix into the vagina.
Endometrial polyps are growths that arise from the inner walls that lined the uterine cavity. It is sometimes called uterine polyps. It is believed to arise from the overgrowth of endometrial tissue. It may range in size from a few millimetres only to a few centimetres. Sometimes, there can be several polyps present at the same time. It may have a long stalk and can extends through the cervix into the vagina.
An endometrial polyp is usually a non-cancerous growth. However, in a small proportion of women, some of these polyps can lead to cancer (called pre-cancerous type). The risk of cancer in a polyp is increased in post-menopausal women. It can arise at any age but rarely occur in women under 20 years old.
Cause and risk factors
The exact cause for the endometrial polyp formation is not well established. The presence of oestrogen hormone is important, which stimulate the endometrium to grow and this has been associated with the growth of the polyps. Your chances of developing endometrial polyps may increase if you are:
- Overweight or obese.
- Taking tamoxifen: this is a drug therapy given for breast cancer treatment.
Symptoms and signs
 Many women with endometrial polyps do not have any symptoms at all. Therefore, in some cases, the diagnosis is then made from a routine pelvic ultrasound scan. Common presentations are:
Many women with endometrial polyps do not have any symptoms at all. Therefore, in some cases, the diagnosis is then made from a routine pelvic ultrasound scan. Common presentations are:
- Abnormal uterine bleeding such as heavy menstrual flow, prolonged bleeding, bleeding or spotting between menses.
- Post-menopausal bleeding.
- Difficulty in conceiving
Diagnosis
The diagnosis is usually made from clinical history (your presenting symptoms) and the ultrasound scan of the uterus.
Investigations
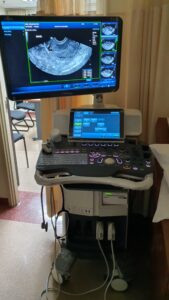
- Pelvic ultrasound scan – this is a procedure in which a handheld device called an ultrasound transducer which emits sound waves is used to provide images of the pelvic organs. It can be done trans-abdominally or trans-vaginally.
Ultrasound scan machine Scan image of endometrial polyp - Saline infusion sonohysterography (SIS) – this is done in combination with the ultrasound scan. Sterile saline fluid is introduced into the uterine cavity through a small catheter. The fluid causes the uterus to expand, providing a clear view of the uterine cavity. Any abnormal structure within the cavity will be seen with the use of the transvaginal pelvic ultrasound scan. The fluid will appear black on scan and the polyp will be seen as a more whitish structure.
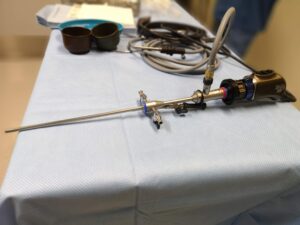
- Hysteroscopy: the hysteroscope is a small lighted telescope used for visual examination of the cervix and the uterus to help diagnose and treat abnormalities in the cervical canal or the uterine cavity. It is inserted into the uterus via the vagina and cervix and enables the doctor to see inside the uterine cavity and locate the endometrial polyp. If it is used to look for the cause of the presenting problem, it is term as diagnostic hysteroscopy. Removal of the polyp can be done at the same time (term as operative hysteroscopy).
Complications
- Difficulty in conceiving – the actual causal relationship is still unclear. The polyp may cause recurrent implantation failure or by mechanical obstruction. Removal of the endometrial polyps has been shown to improve fertility.
- Cancer: Approximately 5 % of endometrial polyps in post-menopausal women can be malignant. In pre-menopausal women, the cancer risk is increased in obese women with irregular and infrequent menses.
Treatment
Treatment will depend on the symptoms, age group, size, risk of malignancy and fertility issues.
1. Conservative – no treatment is required in a young woman who has a small polyp and has no symptoms at all. Some of these small polyps may regress spontaneously.
2. Medications: this is usually given to stop or reduce the abnormal menstrual bleeding due to polyps. Some of these medications are hormonal type (such as progestogens or combined oral contraceptives pills) or non-hormonal (such as tranexamic acids). However, this is usually a temporary measure because the symptoms may recur once the medication is stopped.
3. Surgery will be indicated if
- the endometrial polyp causes symptoms.
- possible risk of malignancy especially if large or rapidly growing.
- a possible cause of difficulty in conceiving.
- If a polyp is discovered after menopause.
The surgical procedure to remove the polyp is called polypectomy and is usually done with a hysteroscope (operative hysteroscopy). An instrument (usually a scissor) is inserted through the hysteroscope to remove the polyps. The removed polyp will be sent for histological evaluation.
Endometrial Curettage – this may be done together with the hysteroscopy. The endometrial lining will be scraped with a curette and this can sometimes remove any small residual polyps.
4. A hysterectomy (surgery to remove the uterus) may be required if the polyp is pre-cancerous or cancerous type.
Prevention
There are no effective methods to prevent endometrial polyps. In women with risk factors such as obesity, infrequent menstrual cycles, abnormal uterine bleeding or taking tamoxifen to treat breast cancer should have regular gynaecological check-ups for early detection. The use of levonorgestrel-releasing intrauterine system or combined oral contraceptives pills in pre-menopausal can be considered if there is an additional need for contraception or treatment of heavy menstrual bleeding.
See your doctor immediately if there is:
- Sudden changes in your menstrual bleeding patterns especially if it becomes heavy and prolonged.
- You feel dizziness, weakness, lethargy, or you feel like you may faint – all these which may suggest the symptoms of anaemia (lack of haemoglobin)
To print a pdf copy, click HERE
[mailerlite_form form_id=3]