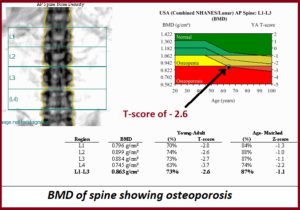
 This test is done to measure the density of bones and this is able to predict the risk of fractures. Bone density decreases in both men and women with age, but in women, the decrease is more rapid and more severe following menopause when the ovaries stop producing the oestrogen hormone. BMD testing can show whether there is significant bone loss, resulting in low bone mass. This is a major cause of osteoporosis and of bone fractures (particularly the hip, spine or forearm) in men and women over the age of 40.
This test is done to measure the density of bones and this is able to predict the risk of fractures. Bone density decreases in both men and women with age, but in women, the decrease is more rapid and more severe following menopause when the ovaries stop producing the oestrogen hormone. BMD testing can show whether there is significant bone loss, resulting in low bone mass. This is a major cause of osteoporosis and of bone fractures (particularly the hip, spine or forearm) in men and women over the age of 40.
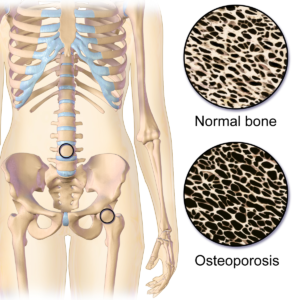
Osteoporosis is a reduction in the amount of bone mass resulting in the loss of bone strength. This will predispose it to fracture. Osteopenia refers to a decrease in bone mineral density and is less severe form compared to osteoporosis. Eventually, it is likely to lead to osteoporosis if no treatment is given.
Reasons for the procedure
- As an aid in diagnosing osteoporosis.

- When X-ray showed evidence suggestive of low bone density.
- Family history of osteoporosis or you have other risk factors for osteoporosis.
- Follow-up of a previous bone-density test to determine the effectiveness of any treatment.
- As a predictor of fracture risks.
- Follow-up testing for women with osteopenia.
- Long-term use of corticosteroids, thyroid hormone, breast cancer drugs, injectable progestogens for contraception such as Depo Provera or anti-epileptics medications – all of these medications can lead to osteoporosis.
Current guidelines now recommend routine screening for all postmenopausal women above the age of 65.
Risk
There are usually no risks associated with this test.
Diet
No special diet is required prior to testing.
Procedure
 Several types of bone density tests are available. The test selected depends on the availability of the equipment. The most accurate, comprehensive and fastest technique is the dual energy x-ray absorptiometry (DXA). This test uses very little radiation. It usually takes only about 5 to 15 minutes to complete. It can measure the bone density of the spine, hip and forearm. This method of testing is the most commonly used and widely available.
Several types of bone density tests are available. The test selected depends on the availability of the equipment. The most accurate, comprehensive and fastest technique is the dual energy x-ray absorptiometry (DXA). This test uses very little radiation. It usually takes only about 5 to 15 minutes to complete. It can measure the bone density of the spine, hip and forearm. This method of testing is the most commonly used and widely available.
Expected Outcome
Tests are completed without any complications. It is non-invasive. The test results will be reported in 2 numbers— the age-matched (called the Z-score) and the young-normal (called the T-score). The Z-score compares your results to other women of the same age as you – a low Z-score (below -2.0) is a warning sign that you have less bone mass than expected for someone your age. The T-score compares your results to a healthy 30-year-old female. The T-score indicate whether your bones are more dense (a plus + sign), or less dense (a minus – sign), or the same density as the healthy 30-year-old female. The reference for interpreting bone mass T-scores are as below:
- Ideal readings = above +1.0 SD (standard deviation).
- Borderline = between a +1.0 SD and a –1.0 SD.
- Osteopenia = between a –1.0 SD and a –2.5 SD.
- Osteoporosis = below a –2.5 SD.
Complications
None is expected from the testing.
 Medication
Medication
You may be prescribed one or more medications or supplements following the test. This will depend on the results and your risk factors for fractures. The medications can be either ac hormone replacement therapy, bone-forming drugs with vitamin D and calcium.
Post-procedure care and activity
 There are no restrictions immediately before or after testing. You can drive or return to work immediately after the test. Exercise is important in developing and maintaining healthy muscle and bone density. Follow a regular fitness program that includes aerobic activity and weight-bearing exercises, such as brisk walking, stair climbing, weight training, etc.
There are no restrictions immediately before or after testing. You can drive or return to work immediately after the test. Exercise is important in developing and maintaining healthy muscle and bone density. Follow a regular fitness program that includes aerobic activity and weight-bearing exercises, such as brisk walking, stair climbing, weight training, etc.
To print a pdf copy, click HERE
To subscribe the newsletter, click HERE